Hey friends, happy Friday.
Most people assume AI will transform healthcare by getting better at diagnosis.
That’s the obvious path.
But it’s not where the most meaningful change is happening.
A different pattern is starting to emerge.
The teams seeing real traction aren’t trying to replace clinicians or outperform them at diagnosis.
They’re focused on something more practical.
Helping healthcare systems make better decisions, faster.
And once you see that, the opportunity shifts.
Because healthcare doesn’t usually break at diagnosis.
It breaks in everything around it.
who gets prioritized
what happens next
how information flows
when decisions are made
That’s where delays creep in.
That’s where inconsistencies show up.
And that’s where most of the system’s inefficiency actually lives.

What we’ll explore today
The big idea: why healthcare is fundamentally a decision system
The shift: how AI is moving from execution to decision-making
Industry breakdown: where AI is already changing real workflows
Case studies: how decision systems are being used today
The data: what the numbers reveal about this shift
Startup opportunities: where builders can create real leverage
Builder playbook: how to approach this space step by step
What this means going forward: how this compounds into system-level change
— Naseema Perveen
OUR 2026 MEDIA KIT IS NOW LIVE
Reach senior decision-makers actually shaping AI adoption, not just browsing the headlines. The AI Journal connects your brand with a global audience of operators and leaders across North America, Europe, and Asia who rely on us for practical, trusted AI insight.
With 484k average monthly unique views, 1.8M total site views in 2025, 154k LinkedIn followers, and nearly 90k newsletter subscribers, your campaigns land in front of an engaged, AI-focused community that cares about outcomes, not hype. If you’re planning thought leadership, product launches, or performance-driven campaigns in AI and enterprise tech, download our 2026 Media Kit today to explore placements that drive real visibility, traffic, and pipeline.
The Big Idea: Healthcare runs on Decisions, not just Expertise
We tend to think of healthcare as expertise-driven.
Doctors diagnose.
Clinicians treat.
But if you zoom out, healthcare is a decision system.
Every outcome depends on a chain of decisions:
Who gets seen first
What path a patient follows
When to escalate care
How resources are allocated
Most systems don’t fail because of lack of expertise.
They fail because of misaligned decisions.
Delays in triage
Poor prioritization
Fragmented coordination
That’s the real bottleneck.
The Data: Where AI is already improving healthcare decisions
It’s easy to talk about this shift conceptually.
But the data points to something very specific:
AI is already delivering value in decision-heavy parts of healthcare, not just automation.
1. Administrative work is the biggest opportunity
According to McKinsey Global Institute:
Generative AI could automate up to 45% of administrative tasks in healthcare
Potential annual value: $150–$260 billion in the U.S. alone
What this means:
→ A large portion of healthcare inefficiency is not clinical
→ It’s coordination, documentation, and workflow decisions
2. Clinicians spend more time on systems than patients
According to American Medical Association:
Physicians spend 2 hours on administrative work for every 1 hour of patient care
What this means:
→ The bottleneck isn’t expertise
→ It’s time lost navigating systems and making fragmented decisions
3. AI is already improving diagnostic decision support
A study published in Nature Medicine found:
AI models can match or exceed human experts in certain diagnostic tasks (e.g., imaging, pathology)
What this means:
→ AI doesn’t need to replace clinicians
→ It can augment high-stakes decisions with better signal detection
4. Better triage leads to better outcomes
Research shows that early warning systems and predictive models can:
detect patient deterioration earlier
reduce ICU transfers
improve survival rates
What this means:
→ The biggest gains often come from earlier decisions, not better treatments
5. Healthcare inefficiency is massive
According to World Economic Forum:
Up to 20–30% of global healthcare spending is wasted due to inefficiencies
What this means:
→ Even small improvements in:
prioritization
coordination
decision timing
→ can unlock massive system-level value
The pattern
Across all of this, a clear pattern emerges:
AI reduces time to insight
AI improves prioritization
AI supports better decisions
Not by replacing humans.
But by improving:
→ when decisions are made
→ what information they’re based on
→ how consistently they’re made
Why this matters
Healthcare doesn’t improve through one breakthrough.
It improves when:
decisions happen earlier
decisions happen faster
decisions happen with better context
And that’s exactly where AI is starting to deliver value today.
The Shift: AI is moving into the decision layer
Healthcare has already improved execution:
electronic health records
standardized workflows
better tools
But execution was never the hardest part.
Decision-making was.
What’s changing now is subtle:
AI isn’t just helping people do work faster.
It’s starting to influence:
what gets prioritized
what gets recommended
what happens next
That might sound incremental.
It isn’t.
Because small improvements in decisions compound into large changes in outcomes.
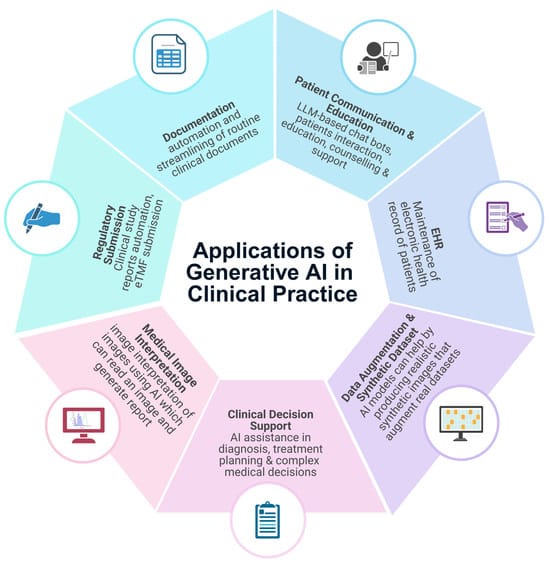
Where this is already happening
Let’s make this concrete.
1. Triage and prioritization
In many hospitals, the challenge isn’t diagnosis.
It’s deciding who needs attention first.
Some hospitals now use AI systems to:
flag high-risk patients
predict deterioration hours earlier
dynamically adjust priority queues
This doesn’t replace clinicians.
It changes how attention is distributed.
And attention is one of the scarcest resources in healthcare.
2. Pre-visit intelligence
Before a consultation, clinicians often spend time:
reviewing patient history
scanning reports
piecing together context
New tools are starting to:
summarize patient records
highlight relevant signals
surface risks ahead of time
Small change.
But it compresses one of the most repetitive decision loops in healthcare.
3. Treatment pathway support
Choosing what to do next is rarely obvious.
AI systems are increasingly used to:
suggest treatment options
compare outcomes
flag inconsistencies
The doctor still decides.
But the system reduces uncertainty.
And in healthcare, reducing uncertainty is everything.
4. Operations and patient flow
This is the least visible layer.
And often the most broken.
Hospitals constantly struggle with:
scheduling
bed allocation
staff coordination
Some systems now:
predict patient inflow
optimize schedules
reduce idle capacity
Most people don’t notice this layer.
But this is where a lot of the system inefficiency lives.
The pattern (once you see it, it’s obvious)

You can map the shift like this:
Execution → already systematized
Diagnosis → partially AI-assisted
Decision-making → now being transformed
The middle layer is where things are breaking open.
Because:
it’s repeated constantly
it’s context-heavy
it’s still largely manual
That combination creates opportunity.
Where startups are getting it wrong
Most founders gravitate toward:
“Let’s build an AI doctor.”
It’s intuitive.
It’s also one of the hardest paths:
heavy regulation
high trust barriers
long sales cycles
A more practical approach is less visible.
And more powerful.
Where startups can actually win
1. Decision support, not replacement
Build tools that:
assist clinicians in real time
surface the right information at the right moment
reduce cognitive load
The goal isn’t to replace judgment.
It’s to improve it.
2. Workflow orchestration
Healthcare systems are fragmented.
Information lives in different places.
Teams operate in silos.
There’s a real opportunity to:
connect systems
automate coordination
reduce handoffs
Most systems don’t fail because they lack intelligence.
They fail because nothing is connected.
3. Risk and prioritization engines
One of the highest-leverage areas:
predicting which patients need attention
identifying early warning signals
enabling earlier intervention
Better prioritization often matters more than better diagnosis.
4. Operational intelligence
This is where many of the fastest wins are.
Tools that:
optimize scheduling
improve capacity planning
reduce bottlenecks
These systems don’t look flashy.
But they create immediate value.
What this means going forward
The future of healthcare likely won’t arrive as a single breakthrough moment.
No headline that says, “AI just fixed healthcare.”
Instead, it will show up in ways that are easy to overlook:
a triage system that flags risk a few hours earlier
a clinician who makes a decision with better context
a hospital that runs slightly more efficiently than before
None of these feel transformational on their own.
But that’s the point.
Healthcare is not a system that changes through big leaps.
It changes through thousands of small decisions getting slightly better.
And once those improvements start to stack, something more interesting happens.
delays shrink
errors decrease
outcomes become more consistent
systems become more responsive
Not because any single part was reinvented.
But because the decision layer underneath everything got stronger.
This is easy to underestimate.
Most people look for visible innovation:
new devices
new drugs
new procedures
But in many cases, the biggest gains won’t come from new capabilities.
They’ll come from better coordination of what already exists.
And that shifts where value is created. It moves away from doing more work or adding more resources, and toward making better decisions at the right time with the right context.
Over time, this creates a widening gap between systems that still rely on manual coordination, delayed decisions, and fragmented information, and those that operate more like continuous decision engines, constantly updating and improving.
At first, the difference is subtle, but as these advantages compound, the gap becomes structural and increasingly difficult to close.
Case studies: Where AI is already changing decisions in healthcare
It’s easy to talk about “AI in healthcare” in abstract terms.
But the more useful lens is this:
Where is AI already influencing real decisions, in real workflows?
Here are a few examples that show how this shift is actually playing out.
1. Sepsis prediction in hospitals
One of the hardest problems in healthcare is catching deterioration early.
Sepsis, for example, can escalate quickly.
And early intervention often determines outcomes.
Hospitals are now using AI systems to:
analyze patient vitals in real time
detect early warning signals
alert clinicians before visible symptoms fully develop
What changed:
The system doesn’t diagnose.
It changes a decision:
→ “Should we intervene now or wait?”
That decision used to rely heavily on experience and timing.
Now it’s supported by continuous monitoring and pattern detection.
2. Radiology workflows (AI-assisted imaging)
Radiologists don’t just read images.
They prioritize:
which scans to review first
which cases are urgent
where to focus attention
AI tools are now being used to:
flag abnormal scans
prioritize high-risk cases
assist with interpretation
What changed:
The core job didn’t disappear.
But the decision of:
→ “What should I look at first?”
became optimized.
And that directly affects speed and outcomes.
3. Clinical documentation and pre-visit summaries
Before a patient interaction, clinicians spend time:
reviewing notes
scanning records
piecing together context
New AI tools are helping by:
summarizing patient histories
extracting key signals
highlighting relevant risks
What changed:
Instead of spending time gathering information, clinicians start with context.
The decision:
→ “What matters in this case?”
becomes faster and more informed.
4. Hospital operations and bed management
Hospitals constantly deal with capacity constraints:
limited beds
fluctuating patient inflow
staff availability
AI systems are now being used to:
predict patient admissions
optimize bed allocation
improve discharge timing
What changed:
This is not a clinical decision.
But it’s still critical.
The system improves:
→ “Who should be admitted, moved, or discharged next?”
Small improvements here unlock massive efficiency.
5. Preventive care and risk scoring
Healthcare is shifting from reactive to proactive.
Some systems now:
analyze patient data continuously
identify high-risk individuals
trigger early interventions
For example:
predicting likelihood of readmission
flagging chronic disease risks
recommending follow-ups
What changed:
Instead of reacting after something happens, the system influences:
→ “Should we act before this becomes a problem?”
That shift moves decisions earlier, where they have more impact.
The takeaway
Across all these examples, the pattern is consistent.
AI is not replacing healthcare professionals.
It’s changing:
what gets prioritized
what gets surfaced
what gets decided
What’s Your Take? — Here’s Your Chance to Be Featured in the AI Journal
What becomes the defining skill in healthcare: expertise, or judgment under uncertainty?
We’d love to hear your perspective.
Email your thoughts to: [email protected]
Selected responses will be featured in next week’s edition.
Builder Playbook: How to Approach This

Healthcare AI does not reward ambition on day one.
It rewards precision.
The teams that win in this space are not the ones with the boldest ideas.
They are the ones who understand how decisions actually get made on the ground and improve them systematically.
Step 1: Find a decision that happens 100+ times a day
Avoid rare edge cases.
Avoid “breakthrough” problems.
Focus on boring, repeated decisions.
Examples:
which patient gets seen next
which appointment gets prioritized
whether a patient is ready for discharge
how a case gets escalated
These decisions don’t look exciting.
But they happen constantly.
And that’s where leverage lives.
Healthcare value is not created by solving rare problems.
It is created by improving decisions that happen thousands of times.
A small improvement in a high-frequency decision will outperform a perfect solution to a low-frequency one.
Step 2: Understand what makes that decision hard
Before building anything, the workflow needs to be understood in detail.
Most healthcare decisions are not difficult because they are complex.
They are difficult because the system around them is fragmented.
Look for three patterns:
Missing context
The decision-maker does not have full visibility.
patient history is scattered
notes are incomplete
data arrives late
Time pressure
Decisions are made quickly, often under stress.
emergency environments
overloaded staff
constant interruptions
Inconsistent outcomes
Two experienced professionals may reach different conclusions.
variability in judgment
lack of standardization
unclear thresholds
If a decision feels messy, ambiguous, and stressful, it is a strong signal.
Clean problems are usually already solved.
Messy decisions are where the opportunity exists.
Step 3: Start with one narrow workflow
Most teams fail by trying to build horizontal solutions too early.
“AI for healthcare decision-making” is too broad to succeed.
Instead, focus on one clearly defined workflow:
ER triage for a specific condition
appointment prioritization in one department
discharge decisions for a defined patient group
The objective is not immediate scale.
The objective is:
clear inputs
clear outputs
measurable impact
Narrow scope creates clarity.
Clarity creates speed.
Once a single workflow works reliably, expansion becomes significantly easier.
Step 4: Design for trust, not autonomy
Healthcare systems do not adopt black-box automation.
They adopt systems they trust.
The goal is not to replace decisions.
The goal is to support decisions.
That requires:
transparent reasoning
surfaced evidence, not just outputs
easy overrides
seamless integration into existing workflows
The system should feel like a second layer of thinking, not a replacement.
In healthcare, trust is not a feature.
It is the product.
Step 5: Build feedback loops early
The first version of any system will be imperfect.
What matters is how quickly it improves.
From day one, capture:
the recommendation made
the decision taken
the outcome observed
This creates a loop:
recommendation → human decision → outcome → system improvement
Over time, the system becomes:
more accurate
more reliable
more trusted
The long-term advantage is not the model.
It is the data generated from real decisions over time.
Step 6: Measure what actually matters
Many teams optimize for technical metrics:
model accuracy
prediction scores
benchmark performance
But healthcare value is created elsewhere.
The correct metrics are:
time saved
errors reduced
outcomes improved
decisions made faster
Even a 10% improvement in a high-frequency decision can create outsized impact.
Step 7: Expand from decisions to systems
Once a single decision is improved, the opportunity expands naturally.
Because decisions are interconnected:
triage influences diagnosis
diagnosis influences treatment
treatment influences outcomes
The path forward:
start with one decision
expand to adjacent decisions
connect them into a system
This is how products evolve from:
→ a tool
→ to infrastructure
The meta insight
Healthcare AI is often framed as an intelligence problem.
It is not.
It is a decision problem.
The real questions are:
where do decisions break
how often do they occur
how much can they be improved
Improving a decision that happens hundreds of times a day, even slightly, is enough to build something valuable.
Closing thought for builders
The starting point is not:
“What can AI do?”
It is:
“What decisions are being made every day that still feel slow, fragmented, or inconsistent?”
That is the entry point.
That is where the next generation of healthcare companies will be built.
What this means going forward
The future of healthcare likely won’t arrive as a single breakthrough moment.
No headline that says, “AI just fixed healthcare.”
Instead, it will show up in ways that are easy to overlook:
a triage system that flags risk a few hours earlier
a clinician who makes a decision with better context
a hospital that runs slightly more efficiently than before
None of these feel transformational on their own.
But that’s the point.
Healthcare is not a system that changes through big leaps.
It changes through thousands of small decisions getting slightly better.
And once those improvements start to stack, something more interesting happens.
delays shrink
errors decrease
outcomes become more consistent
systems become more responsive
Not because any single part was reinvented.
But because the decision layer underneath everything got stronger.
This is easy to underestimate.
Most people look for visible innovation:
new devices
new drugs
new procedures
But in many cases, the biggest gains won’t come from new capabilities.
They’ll come from better coordination of what already exists.
And that shifts where value is created.
From:
doing more work
adding more resources
To:
making better decisions
at the right time
with the right context
Over time, this creates a gap.
Between systems that still rely on:
manual coordination
delayed decisions
fragmented information
And systems that operate more like:
continuous decision engines
constantly updating
constantly improving
That gap will compound.
And it will become very hard to close.
Final thought
Healthcare doesn’t have an intelligence problem.
It has a decision problem.
The expertise already exists.
The data already exists.
What’s been missing is the ability to:
connect it
interpret it
act on it consistently
The teams that understand this shift early won’t just build better tools.
They’ll build the layer that decides:
what happens
when it happens
and how the system responds
And over time, that layer becomes the system itself.
—Naseema
Writer & Editor, AIJ Newsletter
Before You Go
Stay ahead of where AI and technology are actually heading, not just where headlines point.
→ Read deeper insights on AI Journal
→ Explore broader tech coverage on Silicon Valley Journal
Where do you think AI will create the most impact in healthcare first?
That’s all for now. And, thanks for staying with us. If you have specific feedback, please let us know by leaving a comment or emailing us. We are here to serve you!
Join 130k+ AI and Data enthusiasts by subscribing to our LinkedIn page.
Become a sponsor of our next newsletter and connect with industry leaders and innovators.


